Can Poor Gut Health Cause Acne? What the Research Actually Says
You have tried the creams. You have changed your cleanser. You have gone through phases of cutting out chocolate, then dairy, then everything remotely enjoyable. And yet the breakouts keep coming back — sometimes worse, sometimes unpredictably, and rarely in a pattern that makes complete sense.
What most dermatology advice still does not lead with is this: your skin does not operate in isolation. The state of your gut — specifically the trillions of microorganisms living in your digestive system — has a meaningful and increasingly well-documented influence on whether your skin is clear, inflamed, or chronically breaking out.
This is not a fringe wellness theory. The gut-skin axis is now one of the most active research areas in dermatology, with a growing body of peer-reviewed evidence linking gut dysbiosis (an imbalance in gut bacteria) to acne vulgaris. This article explains what that connection actually looks like, the mechanisms behind it, and what you can realistically do about it.
The Research Is Clearer Than You Might Think
Scientists have suspected a gut-skin connection for much longer than the current wave of research suggests. In 1930, dermatologists Stokes and Pillsbury proposed that emotional stress could alter gut bacteria, increase intestinal permeability, and contribute to skin inflammation — a hypothesis that was ahead of its time by nearly a century.
What has changed is the quality of evidence. A 2022 review published through PMC/NIH examining acne, the microbiome, and probiotics found that people with acne consistently show reduced gut microbiome diversity compared to clear-skinned controls. In a study of 114 acne patients, 54% had measurable gut dysbiosis. Another study of 300 acne patients found that 61% had a diagnosis of irritable bowel syndrome — a rate significantly higher than in the general population.
A 2024 clinical review on lifestyle and microbiome influences published in the American Journal of Lifestyle Medicine confirmed a causal relationship between gut microbiota dysbiosis and immune-mediated skin conditions including acne, with researchers using Mendelian randomization methods — a more rigorous form of causal analysis than standard observational studies.
The evidence does not suggest that fixing your gut will cure all acne for everyone. Acne is multifactorial — hormones, genetics, and skin microbiome all play roles. But for a significant proportion of people with persistent or adult-onset acne, gut health is a contributing factor that is rarely addressed in standard skincare routines.
New research is turning the tables. Your gut, and the food you put in it, could influence acne after all. The gut microbiome plays an essential role in regulating both immunity and inflammation — and both of those systems are directly involved in acne development.
Dr. M. Elizabeth Swenor, D.O., Henry Ford Health, November 2025What Is the Gut-Skin Axis?
The gut-skin axis refers to the bidirectional communication network between your gastrointestinal tract and your skin. They are not separate systems operating independently — they share immune pathways, respond to the same inflammatory signals, and are both regulated by microbial communities that interact with each other.
Your gut houses approximately 70% of your body’s immune cells. It also produces more than 30 hormone-like compounds including short-chain fatty acids (SCFAs), cortisol precursors, and neurotransmitters like serotonin and GABA. According to a narrative review on the gut-skin axis published in PMC, disruptions in gut homeostasis — including dysbiosis and increased intestinal permeability — are increasingly recognised as contributing factors in dermatological conditions including acne, psoriasis, and atopic dermatitis.
The communication runs in both directions. Gut dysbiosis can worsen skin inflammation. And skin inflammation, in turn, can impair intestinal barrier function. This bidirectional loop is one reason why people with chronic acne sometimes also report digestive symptoms — and why treating one without addressing the other often produces incomplete results.

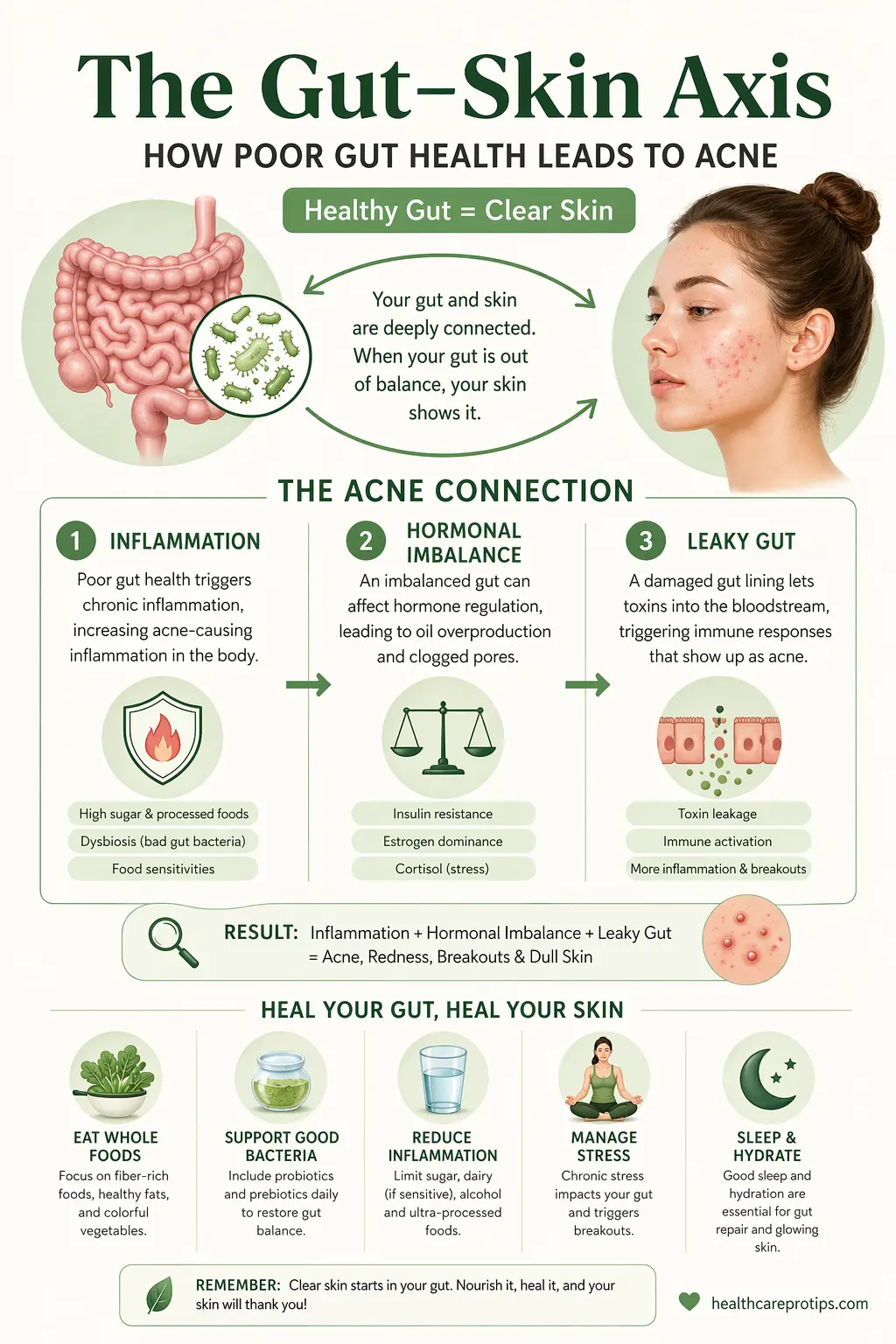
How Poor Gut Health Triggers Acne — The Mechanisms
Understanding exactly how the gut influences your skin makes it far easier to know what to target. There are four primary pathways through which gut dysfunction contributes to acne.
1. Systemic Inflammation
When gut bacteria are imbalanced, harmful bacterial species produce lipopolysaccharides (LPS) — inflammatory compounds that can pass through a compromised gut lining into the bloodstream. Once in circulation, LPS triggers an immune response that sends pro-inflammatory signals throughout the body, including to the skin. This systemic low-grade inflammation is a well-established driver of acne — it activates sebaceous glands, increases sebum production, and creates exactly the conditions in which acne-causing bacteria thrive on the skin surface.
2. Leaky Gut and Increased Intestinal Permeability
A healthy gut lining acts as a selective barrier — allowing nutrients in while keeping bacteria, toxins, and partially digested food particles out of the bloodstream. When gut dysbiosis persists, the tight junctions between intestinal cells can loosen, creating a more permeable gut wall. This condition is commonly called leaky gut.
The result: bacterial byproducts, food antigens, and toxins enter circulation at higher rates, provoking an immune reaction that can express itself as skin inflammation. Research has shown that people with acne have measurably higher markers of intestinal permeability than clear-skinned controls, suggesting that a compromised gut barrier is not an incidental finding in acne patients — it may be a contributing cause.
3. Hormonal Disruption
Your gut microbiome plays a direct role in metabolising hormones, particularly oestrogen and androgens. Gut bacteria produce enzymes that regulate how hormones are recycled and eliminated. When gut bacteria are imbalanced, this hormonal metabolism becomes dysregulated. Androgens — the hormones most directly associated with sebum production and acne — can become elevated when gut bacteria do not metabolise them efficiently.
This is why hormonal acne that clusters around the chin, jaw, and lower cheeks — typically attributed to androgen fluctuations — does not always resolve with hormonal treatments alone. If the underlying gut dysbiosis driving androgen excess is not addressed, the hormonal imbalance tends to persist or return.
4. Reduced Short-Chain Fatty Acids (SCFAs)
Beneficial gut bacteria ferment dietary fibre to produce SCFAs — particularly butyrate, propionate, and acetate. These compounds are essential for maintaining the integrity of both the gut lining and the skin barrier. They regulate immune responses, reduce systemic inflammation, and help keep both barriers intact. When gut dysbiosis reduces SCFA production, the protective effects on the gut and skin are weakened simultaneously, creating conditions more favourable to both leaky gut and inflammatory skin conditions including acne.

Signs Your Acne Might Be Gut-Related
Not all acne is gut-related. But if several of the following patterns apply to you, gut health is worth investigating as part of your approach — something that is consistently underutilised in conventional acne management, as noted in a 2025 report from Henry Ford Health.
- Acne that worsens after certain meals, particularly high-sugar or processed food
- Breakouts accompanied by bloating, irregular bowel movements, or digestive discomfort
- Acne that flares significantly during periods of stress
- Acne that appeared or worsened after a course of antibiotics
- Adult-onset acne with no obvious hormonal trigger
- Acne concentrated on the chin, jaw, or lower face
- Skin that also shows signs of eczema, rosacea, or unusual sensitivity
- Acne limited to the forehead with no digestive symptoms
- Breakouts clearly linked to a specific topical product
- Acne that resolves completely with standard topical treatments
- Teenage acne with no accompanying digestive issues
- Acne that responds predictably to hormonal treatment alone
If you also experience persistent bloating or heaviness alongside your skin concerns, these two issues may share a common root. Our article on why your stomach feels heavy and bloated covers what that gut-level disruption actually looks like and what tends to drive it.
Foods That Trigger Both Gut and Skin Problems
One of the clearest practical applications of the gut-skin axis is understanding that certain foods damage both your gut microbiome and your skin simultaneously through the same inflammatory pathways. This means that changing what you eat can address both issues at once rather than requiring separate skin and gut interventions.
| Food / Category | Effect on Gut | Effect on Skin / Acne |
|---|---|---|
| Refined sugar and sugary drinks | Feeds harmful bacteria, promotes dysbiosis | Spikes insulin, increases androgen production and sebum |
| Ultra-processed foods | Reduces microbiome diversity, promotes inflammation | Drives systemic inflammation that worsens acne |
| Conventional dairy (milk, ice cream) | Can disrupt gut bacteria in lactose-sensitive individuals | Associated with increased IGF-1 and androgen levels linked to acne |
| High-glycaemic carbohydrates | Rapid glucose spikes alter microbiome composition | Elevated insulin stimulates oil glands and inflammatory pathways |
| Alcohol | Depletes beneficial bacteria, increases intestinal permeability | Increases systemic inflammation that can trigger breakouts |
For a more detailed look at which foods are most damaging to the gut microbiome and why, our article on the worst foods for gut health covers the mechanisms and the specific dietary patterns to address.

What You Can Do to Improve Both Gut Health and Acne
The good news about the gut-skin connection is that improving your gut health does double duty. The same dietary and lifestyle changes that rebuild your microbiome also reduce systemic inflammation, regulate hormones, and create conditions where clearer skin becomes more achievable. Here is what the evidence supports.
Increase Dietary Fibre and Plant Diversity
Fibre feeds the beneficial bacteria that produce SCFAs — the compounds that protect both your gut lining and your skin barrier. Aim for a wide variety of plant foods rather than relying on a single fibre source. Different bacteria eat different plants, so variety directly translates to greater microbiome diversity, which is consistently associated with healthier skin outcomes.
Add Fermented Foods Consistently
Plain yoghurt, kefir, kimchi, sauerkraut, and miso introduce live beneficial bacteria into your gut. Clinical studies have shown that probiotic supplementation can reduce acne lesion counts, reduce inflammatory markers in the skin, and improve skin barrier function. Daily small amounts from food sources are a practical starting point before considering probiotic supplements.
Significantly Reduce Sugar and Ultra-Processed Foods
This is the single most impactful dietary change for both gut health and acne simultaneously. Refined sugar and ultra-processed foods damage the microbiome and drive the insulin and androgen spikes that stimulate excess sebum production. Reducing them is not an all-or-nothing effort — consistent reduction over weeks produces measurable changes in both gut bacterial composition and skin inflammation.
Manage Stress as a Gut-Skin Priority
Stress elevates cortisol, which both disrupts gut microbiome balance and directly stimulates sebum production in the skin. The gut-brain-skin axis — a three-way communication system — means that stress management is not optional if you are addressing gut-related acne. Even brief, consistent practices like 10 minutes of daily deep breathing or regular aerobic exercise measurably reduce cortisol and improve both gut and skin outcomes over time.
Consider a Temporary Dairy Elimination Trial
The dairy-acne link is one of the more consistent dietary associations in acne research. Conventional milk contains IGF-1 and hormonal precursors that stimulate androgen receptors in the skin. For people who are also lactose-sensitive, dairy additionally disrupts gut bacteria. A four to six week dairy elimination followed by a gradual reintroduction can help identify whether dairy is a personal trigger for your acne.
Address Slow Digestion as Part of Your Skin Strategy
When waste moves slowly through the colon, bacterial fermentation continues longer than it should, producing more of the compounds associated with systemic inflammation and gut permeability. Keeping digestion moving efficiently — through adequate fibre, hydration, and post-meal movement — reduces the bacterial byproduct load your gut has to manage. Our guide on how to speed up digestion naturally covers the specific strategies that work best for this.

- Poor gut health can contribute to acne through four main pathways: systemic inflammation, leaky gut, hormonal disruption, and reduced SCFA production
- Research involving over 185,000 acne patients found significant associations between acne and gut conditions including IBS and constipation
- The gut-skin axis is bidirectional — gut dysbiosis worsens skin inflammation, and skin inflammation can further impair gut barrier function
- Foods that damage the gut microbiome — particularly refined sugar, ultra-processed foods, and alcohol — also drive the inflammatory and hormonal pathways behind acne
- Dietary changes that improve the gut microbiome (more fibre, fermented foods, reduced sugar and processed food) consistently produce improvements in both gut symptoms and skin clarity
- Gut-targeted strategies work best as part of a complete acne management approach alongside appropriate skincare and, where needed, medical treatment

